IGF 1 LR3 Capsule, also known as long-chain human insulin-like growth factor capsule, is a capsule formulation product made by processing the highly active peptide substance IGF-1 LR3 modified by genetic engineering as the core raw material, combined with suitable excipients through formulation technology. This dosage form not only retains the core biological activities of IGF-1 LR3, such as promoting cell proliferation and inhibiting apoptosis, but also reduces its damage to the external environment during storage and administration through the protective effect of the capsule shell, and improves the convenience of administration. It has special value in the exploration and application of biomedical research and fitness fields, and its production, application, and control must comply with strict regulations related to biological products. As a peptide substance, it is highly sensitive to temperature, humidity, and proteases in the gastrointestinal tract. Capsule formulations have unique adaptability to it, and compared with freeze-dried powder injections, tablets, and other formulations, they have obvious advantages.
|
|
|

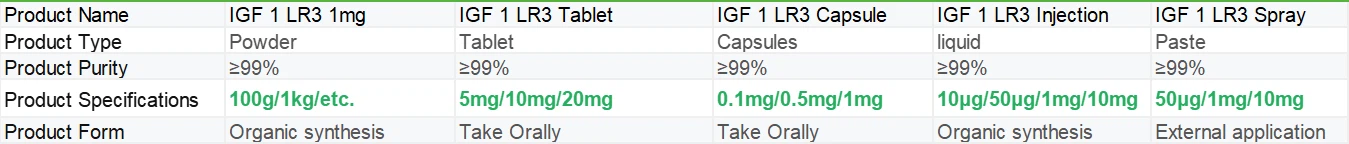
IGF 1 LR3 COA

The effect of IGF-1 LR3 capsule on the physical barrier of intestinal epithelium
As the largest digestive and absorptive organ and immune defense barrier in the human body, the integrity of its epithelial physical barrier directly determines the homeostasis of intestinal function. When the physical barrier of the intestinal epithelium is damaged, intestinal permeability increases, which can easily lead to dysbiosis of the intestinal microbiota, inflammatory reactions, and even systemic diseases. IGF-1 LR3 (long-chain human insulin-like growth factor-1), as a highly active peptide, can be stably released in the intestine and exert biological effects after oral administration in capsule form. In recent years, studies have shown that IGF 1 LR3 Capsule have significant protective and reparative effects on the physical barrier of intestinal epithelium, and their mechanisms involve multiple dimensions such as cell proliferation regulation and tight junction protein expression regulation.
The core function of the physical barrier of intestinal epithelium
The function of the physical barrier of intestinal epithelium can be summarized as two core functions: "selective permeability" and "defensive protection", which work together to maintain the homeostasis of the intestinal environment.
The balance between nutrient absorption and material barrier. Under normal circumstances, the physical barrier of the intestinal epithelium allows small molecule nutrients such as water, electrolytes, and glucose to pass through, while preventing harmful substances such as bacteria, endotoxins, and food antigens from entering the body. This selectivity mainly relies on the "pore size screening" effect of tight junctions: small molecules can be absorbed through the tightly connected "paracellular pathway" or the "transcellular pathway" of epithelial cells; However, large molecular substances are confined within the intestinal lumen due to their inability to pass through tightly connected narrow channels. In addition, surface transporters of epithelial cells, such as glucose transporter GLUT2 and amino acid transporter SGLT1, can specifically transport nutrients, further enhancing the selectivity of permeability.

Defense and protection function
The "first line of defense" intestinal epithelial physical barrier against external invasion resists external invasion through multiple mechanisms: first, the "physical barrier" of the mucus layer. The mucin secreted by the goblet cells forms a gel like mucus layer, which can absorb bacteria and toxins in the intestinal cavity and prevent them from directly contacting epithelial cells; The second is the "sealed defense" of tight junctions, which maintains the low permeability of the barrier and prevents the leakage of harmful substances by regulating the expression and distribution of tight junction proteins; The third is the "active clearance" of epithelial cells, which can engulf small molecules of harmful substances through phagocytosis and degrade them through lysosomes; The fourth is synergistic immune defense. When the barrier is damaged, epithelial cells can secrete cytokines (such as IL-8, TNF - α), recruit immune cells (such as neutrophils, macrophages) to clear pathogens, and repair the barrier damage.
Intestinal absorption characteristics of IGF-1 LR3 (based on capsule formulation)
After oral administration of IGF 1 LR3 Capsule, its absorption process requires overcoming multiple intestinal barriers, including gastric acid, intestinal proteases, and tight junctions between epithelial cells. The design of the capsule formulation provides assurance for the intestinal absorption of IGF-1 LR3:
The protective effect of capsule shell
IGF-1 LR3 capsules often use hydroxypropyl methylcellulose (HPMC) capsule shells, which are insoluble in the stomach (pH 1-3) and can protect IGF-1 LR3 from gastric acid damage; After reaching the intestine (pH 6-7), the capsule shell gradually dissolves and releases the active ingredient. In addition, stabilizers added to the capsule contents, such as mannitol and disodium EDTA, can prevent IGF-1 LR3 from being degraded by proteases in the intestine and maintain its biological activity.


Intestinal absorption pathway
As a polypeptide substance, IGF-1 LR3 is mainly absorbed in the intestine through two pathways: one is the transcellular pathway, where epithelial cells phagocytose IGF-1 LR3 into the cell to form an endosome. Before the endosome fuses with lysosomes, IGF-1 LR3 can be released to the basal side through "exocytosis" and enter the lamina propria or bloodstream; The second is the paracellular pathway, where IGF-1 LR3 can be absorbed in small amounts through the intercellular space by regulating the permeability of tight junctions. Research has shown that after oral administration of IGF-1 LR3 capsules, the local concentration of IGF-1 LR3 in the intestine is significantly higher than that in the blood, indicating that it mainly functions locally in the intestine. This characteristic makes it more suitable for the protection and repair of intestinal epithelial physical barriers.
Factors affecting absorption efficiency
The intestinal absorption efficiency of IGF-1 LR3 is influenced by multiple factors: firstly, the selection of excipients. Solubilizers (such as Tween 80) in the capsule contents can improve the water solubility of IGF-1 LR3 and promote its contact with epithelial cells; The second is the intestinal environment, where dysbiosis and inflammatory reactions can damage epithelial cells and affect absorption efficiency; The third is dosage. At low doses (such as 10-100 μ g/kg), the absorption efficiency is higher, and as the dosage increases, the absorption efficiency gradually saturates. Therefore, in the development of capsule formulations, it is necessary to optimize the prescription and adjust the dosage to ensure that IGF-1 LR3 reaches an effective concentration in the intestine.
The effect of IGF-1 LR3 on the integrity of intestinal epithelial physical barrier
The effect of IGF 1 LR3 Capsule on the integrity of the intestinal epithelial physical barrier has been validated through extensive cell experiments and animal model studies. These studies reveal the protective and reparative effects of IGF-1 LR3 from multiple dimensions such as barrier permeability, tight junction protein expression, epithelial cell proliferation and apoptosis, providing experimental evidence for its application in intestinal diseases.
Cell experiment: Regulatory effect of IGF-1 LR3 on intestinal epithelial cell barrier
Intestinal epithelial cell lines, such as Caco-2 cells and IEC-6 cells, are often used to construct in vitro barrier models. Barrier permeability is evaluated by detecting indicators such as transepithelial electrical resistance (TEER) and fluorescein sodium permeability; By using Western blot, immunofluorescence and other techniques, the expression and distribution of tight junction proteins were analyzed, and the effect of IGF-1 LR3 on barrier integrity was studied.
Reduce barrier permeability and enhance barrier tightness
Caco-2 cells are a type of human colon adenocarcinoma cell that can differentiate into polar columnar epithelial cells when cultured in vitro, forming tight junction structures similar to those in vivo. They are a commonly used model for studying the intestinal epithelial barrier.
Upregulation of tight junction protein expression and improvement of junction structure
The expression and distribution of tight junction proteins are key factors affecting barrier integrity. Multiple cell experiments have shown that IGF-1 LR3 can improve the tight junction structure by upregulating the expression of tight junction proteins such as occludin, ZO-1, claudin-1, etc.
Promote epithelial cell proliferation and inhibit cell apoptosis
The balance between proliferation and apoptosis of intestinal epithelial cells is the basis for maintaining barrier integrity. IGF-1 LR3 can promote cell proliferation, inhibit cell apoptosis, and repair damaged epithelial cell layers.
Animal model: Protection and repair of intestinal epithelial physical barrier by IGF-1 LR3
Animal models are closer to the physiological environment in vivo and can comprehensively evaluate the impact of IGF-1 LR3 on the physical barrier of intestinal epithelium. Common animal models include inflammatory bowel disease (IBD) model, ischemia-reperfusion (I/R) injury model, radiation-induced intestinal injury model, etc. The role of IGF-1 LR3 is validated by detecting pathological changes in intestinal tissue, barrier permeability, tight junction protein expression, and other indicators.
Inflammatory bowel disease (IBD) model: Relieve inflammation, repair barriers
A mouse ulcerative colitis (UC) model induced by DSS (dextran sulfate sodium) was used to simulate intestinal inflammation and barrier damage in human IBD, and the protective effect of IGF-1 LR3 was studied. The experiment was divided into a normal control group, a DSS model group, and a DSS+IGF-1 LR3 treatment group (with doses of 0.1mg/kg, 0.5mg/kg, and 1mg/kg, respectively, orally administered daily), and treated continuously for 7 days.
Ischemia reperfusion (I/R) injury model: reducing ischemic injury and restoring barrier function
Intestinal ischemia-reperfusion injury is common in clinical scenarios such as shock and surgery, which can lead to epithelial cell necrosis and barrier damage. An I/R injury model was established by clamping the mouse mesenteric artery for 30 minutes and reperfusion for 6 hours to investigate the effect of IGF-1 LR3. The experiment was divided into sham surgery group, I/R model group, and I/R+IGF-1 LR3 treatment group (0.5mg/kg, orally administered 30 minutes before reperfusion).
Radiation induced intestinal injury model: promoting mucosal repair and maintaining barrier integrity
Radiation induced intestinal injury is a common complication of abdominal tumor radiotherapy, mainly manifested as intestinal mucosal damage and barrier dysfunction. A radiation-induced intestinal injury model was established by irradiating the abdomen of mice with 60Co gamma rays (dose 10 Gy) to investigate the reparative effect of IGF-1 LR3. The experiment was divided into a normal control group, a radiotherapy model group, and a radiotherapy+IGF-1 LR3 treatment group (1mg/kg, orally taken from the first day after radiotherapy, once a day, for 7 consecutive days).
Hot Tags: igf 1 lr3 capsule, suppliers, manufacturers, factory, wholesale, buy, price, bulk, for sale









