Shaanxi BLOOM Tech Co., Ltd. is one of the most experienced manufacturers and suppliers of exenatide suspension in China. Welcome to wholesale bulk high quality exenatide suspension for sale here from our factory. Good service and reasonable price are available.
Exenatide Suspension is a type of hypoglycemic drug based on glucagon like peptide-1 (GLP-1) receptor agonists, belonging to the peptide class. Its core component, Exenatide, is a peptide composed of 39 amino acids synthesized through genetic recombination technology. The drug was initially jointly developed by Eli Lilly and Amlin Pharmaceuticals, and was approved for market by the US Food and Drug Administration (FDA) in 2005, becoming the first GLP-1 receptor agonist drug.
Our Products Form




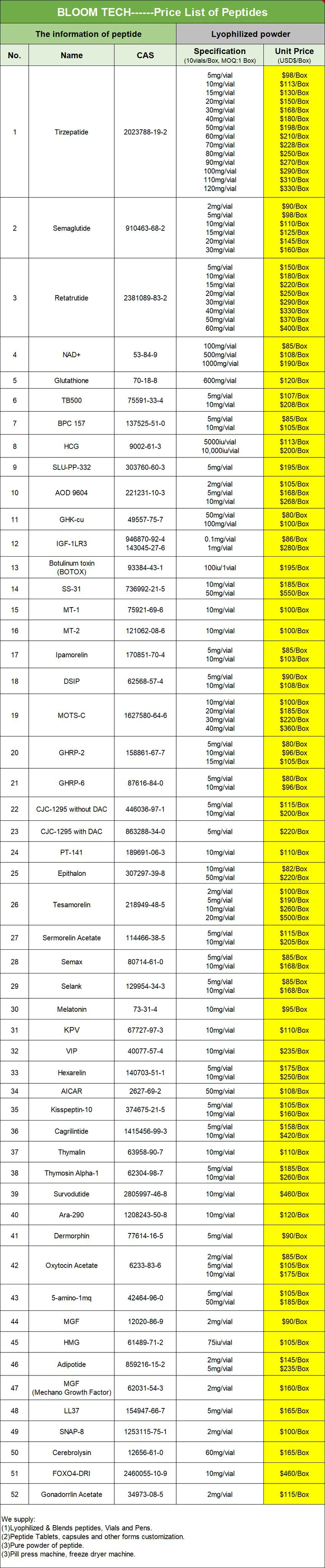
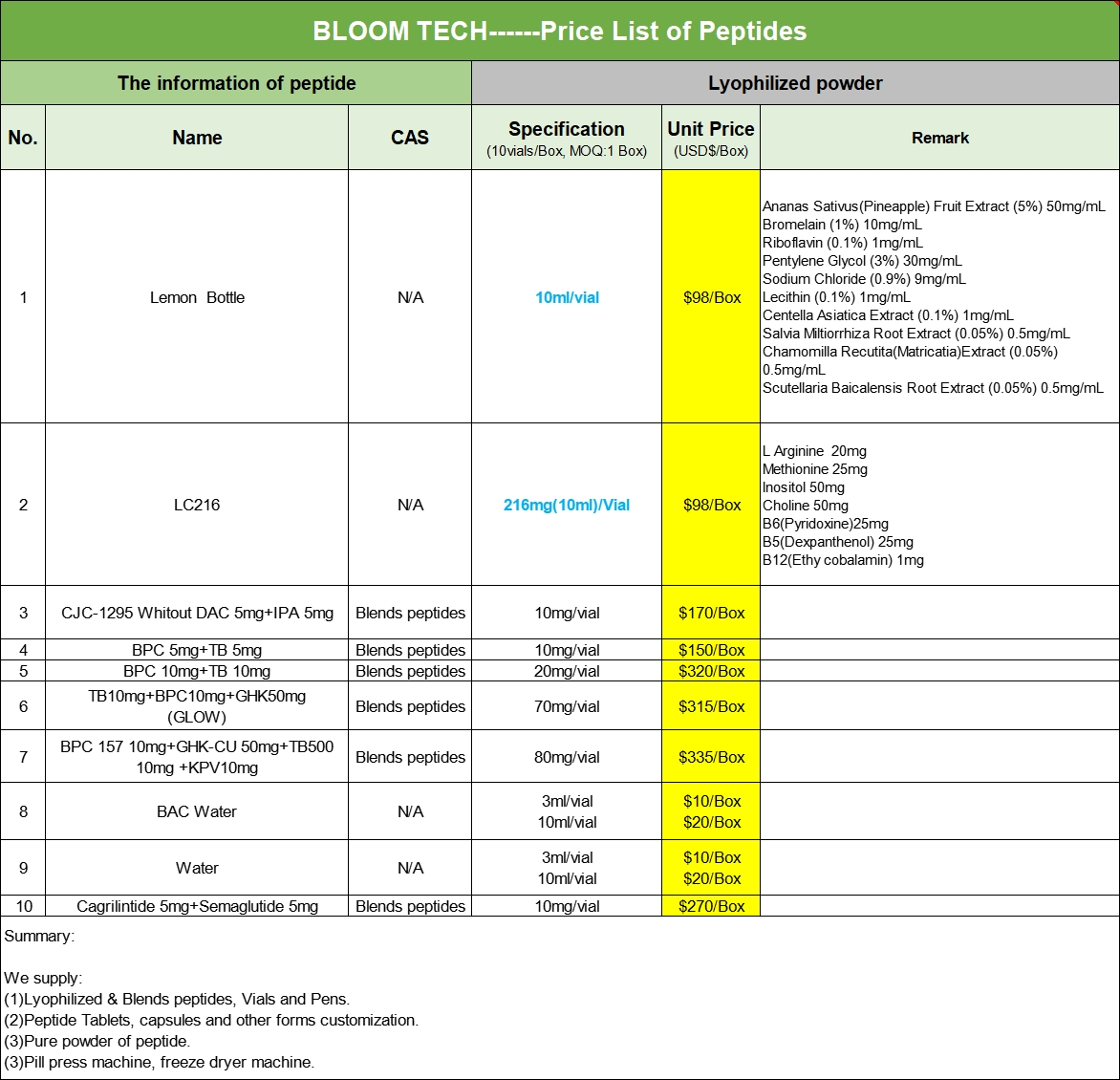

Exenatide/Exenatide acetate COA


Progressive attenuation of islet β cell quality (quantity and function) is the core pathological feature of type 2 diabetes. Pathological factors such as high sugar, lipid toxicity, oxidative stress, inflammation, and endoplasmic reticulum stress inhibit β - cell proliferation and induce β - cell apoptosis, leading to the collapse of functional β - cell populations. Exenatide Suspension, as a classic GLP-1 receptor agonist, activates the three core signaling networks of PI3K Akt, cAMP PKA Epac, and AMPK-SIRT1 downstream of GLP-1 R, achieving triple precision regulation of β - cell quality: promoting pancreatic stem/precursor cell differentiation into β - cells, stimulating mature β - cell proliferation, and effectively inhibiting β - cell apoptosis.
Embryonic development and tissue distribution of beta cells
The development of beta cells originates from the endoderm, and their differentiation and maturation is a multi-stage, multi gene precise regulation process that mainly occurs in the middle and late stages of embryonic development. After birth, there will still be a certain degree of proliferation and maturation.
Formation of pancreatic primordia
During the 3rd to 4th week of embryonic development, the cells of the foregut endoderm differentiate into dorsal and ventral pancreatic buds, which are the embryonic forms of pancreatic development. At this time, endocrine cell differentiation has not yet occurred.


Differentiation of endocrine precursor cells
During the 8th to 10th week of the embryo, the epithelial cells in the pancreatic bud gradually differentiate into multipotent pancreatic precursor cells, which further differentiate into endocrine precursor cells and begin to express pancreatic cell specific transcription factors such as PDX-1, NKX6.1, PAX4, etc. These transcription factors are nuclear regulatory molecules for the directed differentiation of beta cells.
β - cell maturation and pancreatic islet formation
After 12 weeks of embryonic development, endocrine precursor cells gradually differentiate into immature beta cells and begin to express insulin genes; From 20 weeks of gestation until birth, immature beta cells rapidly proliferate, migrate, and aggregate, forming a structurally intact pancreatic islet together with alpha cells, delta cells, and other cells. Beta cells occupy the central position of the pancreatic islet, forming the classic pancreatic islet structure of "central beta cells and peripheral other cells".


Maturation and proliferation after birth
From neonatal period to adolescence, beta cells continue to proliferate and mature, and insulin secretion function gradually improves; After adulthood, the proliferation ability of beta cells significantly decreases, mainly by maintaining a stable cell count. Limited compensatory proliferation may occur when metabolic load increases (such as obesity and pregnancy).
Reference information source:
- Chen Jialun Clinical Endocrinology (2nd edition) Shanghai Science and Technology Press, 2011
- Bonner-Weir S. Life and death of the pancreatic beta cell. Diabetes Science and Technology. 2010.
- Finegood DT, Scaglia L, Bonner-Weir S. Dynamics of beta-cell mass in the growing rat pancreas. Diabetes. 1995.
- Kahn SE, Hull RL, Utzschneider KM. Mechanisms linking obesity to insulin resistance and type 2 diabetes. Nature. 2006.
β cell mass decline: the core pathological driver of type 2 diabetes
Physiological regulation system of β - cell quality
The maintenance of beta cell quality in adult organisms is a dynamic equilibrium process, which is regulated by three core components:
Neogenesis of β - cells: Pancreatic ductal epithelial stem cells, acinar cells, alpha cells, and other precursor cells differentiate into functional β - cells, which are an important source of β - cell supplementation in adulthood.
Proliferation of beta cells: Mature beta cells replicate themselves through mitosis, which is the main pathway for mass expansion of beta cells after birth.


Apoptosis of beta cells: Overactivation under pathological conditions leads to the death and reduction of beta cell numbers.
Under physiological conditions, the three are balanced to maintain a stable population of functional beta cells; In type 2 diabetes, neogenesis and proliferation are inhibited, apoptosis is hyperactive, and balance is completely collapsed.
Glucotoxicity: Chronic high glucose induces oxidative stress, mitochondrial dysfunction, endoplasmic reticulum stress (ERS), and activates JNK, p38 MAPK, and CHOP apoptotic pathways.
Lipotoxicity: Accumulation of free fatty acids (FFA) induces lipid apoptosis, mitochondrial damage, and insulin secretion defects in beta cells.
Oxidative stress outbreak: Excessive generation of ROS, damaging DNA, proteins, and lipids, activating the apoptotic cascade.


Endoplasmic reticulum stress (ERS): Accumulation of unfolded proteins activates the PERK-eIF2 α - ATF4 CHOP pathway, inducing apoptosis.
Inflammatory injury: Chronic low-grade inflammation of the pancreas, where pro-inflammatory factors such as TNF - α, IL-1 β, IFN - γ activate the NF - κ B and Caspase apoptotic pathways.
IAPP abnormal aggregation: pancreatic amyloid peptide misfolded to form toxic oligomers, damaging beta cell membranes and inducing apoptosis.
Reference information source:
- Molecular mechanism study of Exenatide regulating liver circadian rhythm. Chinese Pharmacological Bulletin, 2024
- The GLP-1 receptor agonist, Exenatide, Administration Time Differentially Affects Circadian Rhythms in Diabetic db/db Mice. University of Kentucky College of Medicine, 2024
- The regulatory effect and clinical significance of GLP-1 receptor agonists on liver circadian rhythm. Chinese Journal of Endocrinology and Metabolism, 2024
The receptor and signaling pathway basis of Exenatide regulating β - cell mass
GLP-1R (G protein coupled receptor B family) is highly expressed in pancreatic beta cell membranes and localized on organelle membranes such as endoplasmic reticulum and mitochondria, providing a structural basis for the multidimensional regulation of exenatide suspension.
Cell membrane GLP-1R: initiates intracellular signaling to regulate proliferation and apoptosis.
Cell membrane GLP-1R: directly regulates endoplasmic reticulum and mitochondrial homeostasis, inhibits ERS and oxidative stress.

Exenatide activates the triple regulatory core pathway of GLP-1R

After high affinity binding with GLP-1R, Exenatide activates three major cross synergistic signaling networks, accurately mediating β - cell neogenesis, proliferation, and anti apoptosis:
PI3K Akt-FoxO1 pathway: a core proliferation and anti apoptotic pathway that promotes cyclin D1 expression, inhibits FoxO1, GSK3 β, and pro apoptotic proteins.
CAMP PKA Epac pathway: promotes β - cell regeneration, enhances insulin gene expression, inhibits ERS, and stabilizes mitochondrial membrane potential.
AMPK-SIRT1-PGC-1 α pathway: regulates autophagy, mitochondrial biosynthesis, antioxidant stress, and improves energy metabolism.
The three major pathways mutually enhance each other: Akt activates AMPK, PKA enhances Akt activity, SIRT1 deacetylates FoxO1 and PGC-1 α, forming a comprehensive β - cell protective network.

The structural basis of Exenatide β cell protection

Exenatide (Exendin-4) 39 peptide has beta cell targeting adaptability:
High affinity binding to β - cell GLP-1 R, with an activation efficiency more than 10 times that of natural GLP-1.
Resistant to DPP-4 degradation, with a half-life of 2.4 hours, long-lasting activation of signaling pathways.
Weak positive charge, easily penetrates the β cell membrane, and accumulates in the cytoplasm and organelles.
Reference information source:
- The mechanism by which exenatide inhibits pyroptosis and improves hepatic insulin resistance through PPAR δ inhibition. BioTech, 2026
- Exenatide ameliorates hepatic steatosis and attenuates fat mass and FTO gene expression through PI3K signaling pathway in nonalcoholic fatty liver disease. PMC, 2024
- Exenatide Attenuates Non-Alcoholic Steatohepatitis by Inhibiting the Pyroptosis Signaling Pathway. Frontiers in Endocrinology, 2021
Regulation of β - cell neogenesis: promoting precursor cell transdifferentiation
Adult pancreas contains multipotent precursor cells (ductal epithelium, acini, alpha cells) with a low rate of neogenesis under physiological conditions; The neogenesis of diabetes is inhibited and cannot compensate for the loss of apoptosis. Exenatide effectively activates the regeneration of beta cells and is a key mechanism for supplementing the beta cell population.

Molecular mechanism of Exenatide promoting β - cell neogenesis

Activate pancreatic precursor cell stemness
Pathway: The cAMP PKA CREB and PI3K Akt pathways synergistically activate β - cell specific transcription factors such as Ngn3, Pdx-1, and Nkx6.1.
Effect: The ductal epithelial stem cells undergo dedifferentiation to obtain stemness, initiating the β - cell differentiation program.
Promote the differentiation of alpha cells into beta cells
Mechanism: Upregulation of PCSK1 and Pax4, inhibition of alpha cell marker genes (Arx, Glucagon), and promotion of alpha cell fate transition to beta cells.
Evidence: In db/db mice, Exenatide increases the differentiation rate of alpha cells by 3-4 times, and the proportion of newly generated beta cells reaches 20% -30%.
Regulating the pancreatic microenvironment
Inhibit pancreatic fibrosis and inflammation, improve extracellular matrix (ECM), and provide a suitable microenvironment for angiogenesis.
Upregulation of SDF-1 enhances precursor cell homing and differentiation.
Collaborative regulation of biological clock
Exenatide synchronizes the pancreatic circadian clock, activates CLOCK/BMAL1, and rhythmically enhances the expression of genes related to neogenesis.

Pathological effects of β - cell neogenesis

Animal model: Exenatide treatment of db/db and high-fat fed mice for 8-12 weeks resulted in a 50% to 70% increase in the number of newly generated beta cells and a significant increase in insulin positive cells in the pancreas.
Cell model: Inducing differentiation of human pancreatic ductal cells and iPS cells into beta cells, Exenatide increases differentiation efficiency by over 60%.
Reference information source:
- Molecular mechanism study of Exenatide regulating liver circadian rhythm. Chinese Pharmacological Bulletin, 2024
- The GLP-1 receptor agonist, Exenatide, Administration Time Differentially Affects Circadian Rhythms in Diabetic db/db Mice. University of Kentucky College of Medicine, 2024
- The mechanism by which exenatide inhibits pyroptosis and improves hepatic insulin resistance through PPAR δ inhibition. BioTech, 2026
Frequently Asked Questions
Q: Why does exenatide suspension sometimes cause transient blood glucose elevation immediately after injection?
+
-
A: The microsphere formulation releases a small initial burst of exenatide, which can temporarily slow gastric emptying more strongly and alter early insulin/glucagon dynamics. In some individuals, this transiently raises blood glucose before the stable therapeutic effect takes over.
Q: Can the injection suspension affect skin collagen or elastin locally with long-term repeated use?
+
-
A: Yes. The sustained-release microspheres produce mild chronic local inflammation. Over months, this can subtly alter dermal fibroblast activity, leading to mild localized thickening or reduced skin elasticity at frequent injection sites, which is not seen with immediate-release formulations.
Q: Why is exenatide less affected by renal impairment compared with immediate-release exenatide?
+
-
A: Its continuous low-level release avoids high peak plasma concentrations. Since GLP-1 receptor agonists are cleared partly by the kidney, lower peaks reduce renal filtration load, making it more forgiving in mild to moderate renal dysfunction.
Q: Does the suspension base interfere with common hormone or antibody immunoassays?
+
-
A: The polymer microspheres and suspending vehicle can weakly bind to assay antibodies or cause nonspecific background signal. This may lead to slight underestimation or matrix effects in some immunoassays if not properly accounted for.
Q: Why does exenatide have a lower risk of tachyphylaxis (reduced response over time)?
+
-
A: Stable, continuous receptor stimulation avoids the large concentration fluctuations seen with BID injections. This reduces the frequency of GLP-1 receptor internalization and desensitization, helping preserve glycemic efficacy longer in some patients.
Hot Tags: exenatide suspension, suppliers, manufacturers, factory, wholesale, buy, price, bulk, for sale









