Shaanxi BLOOM Tech Co., Ltd. is one of the most experienced manufacturers and suppliers of octreotide injection 100 mcg in China. Welcome to wholesale bulk high quality octreotide injection 100 mcg for sale here from our factory. Good service and reasonable price are available.
Octreotide Injection 100 mcg is an injection containing Octreotide Acetate, with a specification of 100 micrograms (mcg) of Octreotide Acetate per milliliter. It belongs to prescription drugs and is mainly used to treat specific types of endocrine tumors, acromegaly, and certain acute bleeding conditions. It appears as a colorless or almost colorless clear liquid and is used for subcutaneous injection or intravenous infusion.
Our Products Form




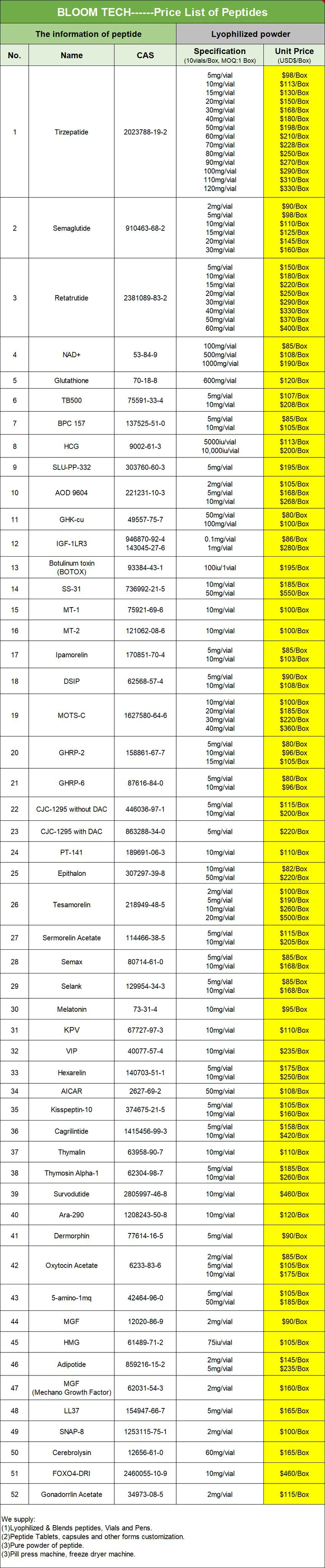
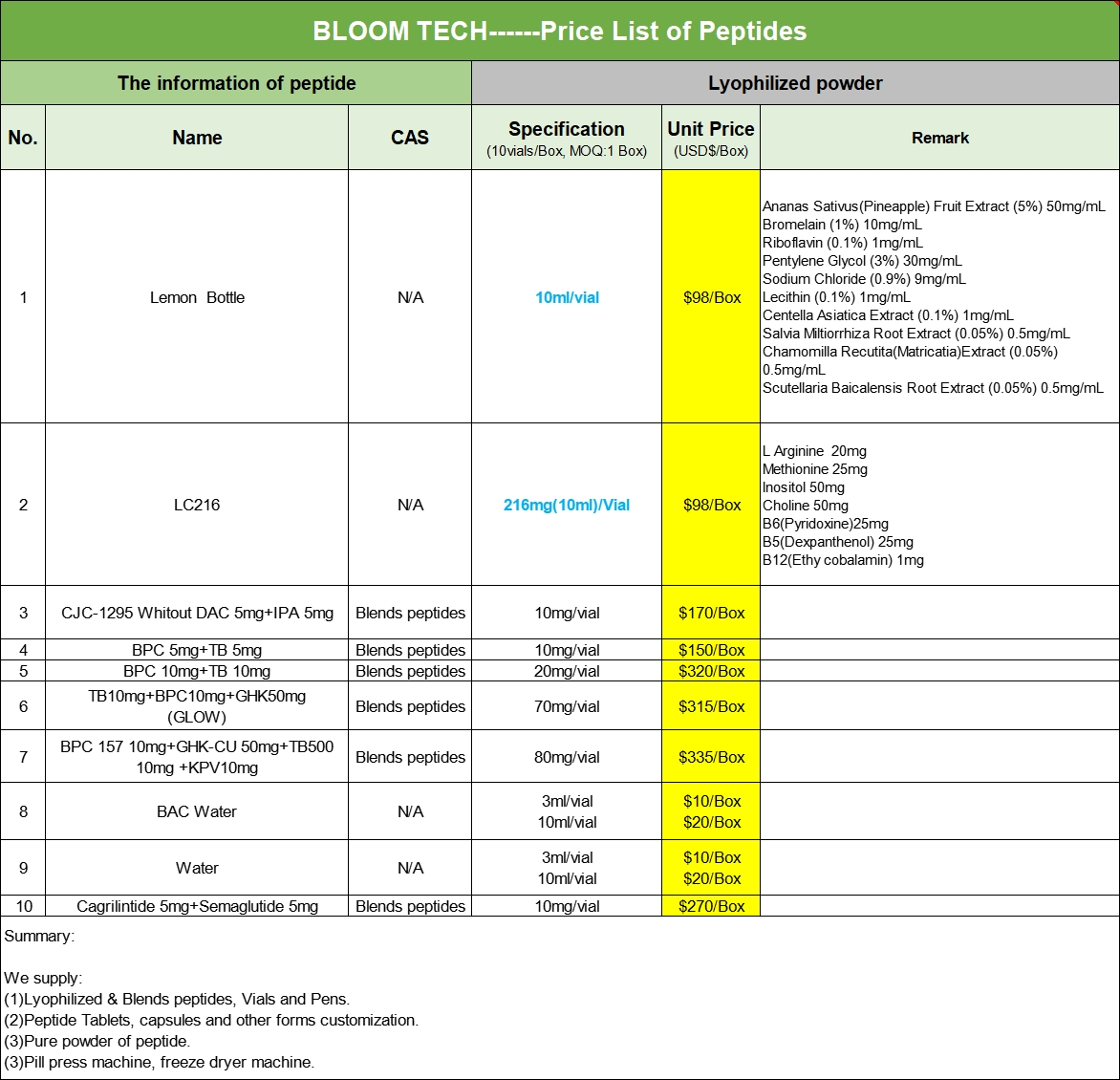

Octreotide COA
 |
||
| Certificate of Analysis | ||
| Compound name | Octreotide | |
| Grade | Pharmaceutical grade | |
| CAS No. | 79517-01-4 | |
| Quantity | Customize | |
| Packaging standard | Customize | |
| Manufacturer | Shaanxi BLOOM TECH Co., Ltd | |
| Lot No. | 202601090055 | |
| MFG | Jan 9th 2026 | |
| EXP | Jan 8th 2029 | |
| Structure |
|
|
| Item | Enterprise standard | Analysis result |
| Appearance | White or almost white powder | Conformed |
| Water content | ≤5.0% | 0.48% |
| Loss on drying | ≤1.0% | 0.30% |
| Heavy Metals | Pb≤0.5ppm | N.D. |
| As≤0.5ppm | N.D. | |
| Hg≤0.5ppm | N.D. | |
| Cd≤0.5ppm | N.D. | |
| Purity (HPLC) | ≥99.0% | 99.90% |
| Single impurity | <0.8% | 0.56% |
| Total microbial count | ≤750cfu/g | 170 |
| E. Coli | ≤2MPN/g | N.D. |
| Salmonella | N.D. | N.D. |
| Ethanol (by GC) | ≤5000ppm | 400ppm |
| Storage | Store in a sealed, dark, and dry place below -20°C | |
|
|
||
|
|
||
| Chemical Formula: | C49H66N10O10S2 |
| Exact Mass: | 1018.44 |
| Molecular Weight: | 1019.25 |
| m/z: | 1018.44(100.0%),1019.44(53.0%),1020.45(13.8%),1020.44(9.0%),1021.44(4.8%),1019.44 (3.7%),1020.44(2.1%),1020.44(2.0%),1019.44(1.6%),1021.45(1.5%),1022.44(1.2%),1021.45(1.1%) |
| Elemental Analysis: | C,57.74;H,6.53;N,13.74;O,15.70;S,6.29 |

As the core organ of the human digestive system, the pancreas secretes pancreatic enzymes to break down fats, proteins, and carbohydrates in food. However, in pathological conditions such as chronic pancreatitis (CP), insufficient pancreatic enzyme secretion (pancreatic enzyme silencing) and impaired fat absorption (fat diarrhea) form a vicious cycle, leading to a deterioration of the patient's nutritional status. Octreotide Injection 100 mcg, as an artificially synthesized somatostatin analog, attempts to break this pathological chain by inhibiting pancreatic enzyme secretion, regulating gastrointestinal motility, and hormone levels. However, there is controversy over its mechanism of action and clinical efficacy, especially in the complex phenomenon of "misalignment" of the digestive timeline.
The pathological basis of pancreatic enzyme silencing: from insufficient secretion to feedback imbalance
Pancreatic enzyme secretion is regulated by both neural and humoral pathways:
Neuroregulation: The vagus nerve directly stimulates pancreatic acinar cells to secrete pancreatic enzymes through acetylcholine;
Fluid regulation: Cholecystokinin (CCK) and secretin are the main hormone regulatory factors. CCK is secreted by I cells in the duodenal and jejunal mucosa, and its release is stimulated by fats and proteins in food. By activating CCK receptors on the surface of pancreatic acinar cells, it promotes the synthesis and secretion of pancreatic enzymes (such as pancreatic lipase and trypsin).

The mechanism of pancreatic enzyme silencing in CP patients

In CP, pancreatic tissue fibrosis leads to a decrease in the number of acinar cells and a decrease in pancreatic enzyme secretion ability. But more importantly, there is feedback regulation imbalance:
Abnormal accumulation of CCK releasing peptide (CCK-RP): Under normal physiological conditions, trypsin in the duodenum can degrade CCK-RP, thereby inhibiting excessive release of CCK. Due to insufficient secretion of pancreatic enzymes, CP patients experience reduced degradation of CCK-RP, resulting in sustained high-level stimulation of the pancreas by CCK, forming a vicious cycle of "insufficient secretion of pancreatic enzymes → elevated CCK → excessive stimulation of the pancreas → further damage".
Negative feedback failure of pancreatic enzyme secretion: Non enteric trypsin preparations (such as Viokase-16) can degrade CCK-RP and reduce CCK levels by supplementing pancreatic protease in the duodenum, thereby relieving pain. However, enteric coated preparations cannot effectively inhibit CCK due to the release of pancreatic enzymes in the jejunum or ileum, resulting in poor therapeutic efficacy.

Misalignment of the digestion timeline of pancreatic enzyme silencing

During normal digestion, the secretion of pancreatic enzymes synchronizes with the entry of food into the duodenum, forming a time axis matching "eating CCK release pancreatic enzyme secretion fat digestion". CP patients may experience delayed or insufficient secretion of pancreatic enzymes, leading to:
Delayed fat digestion: Insufficient concentration of pancreatic lipase in the duodenum hinders fat emulsification and hydrolysis;
Acidic environment inhibits pancreatic enzyme activity: Patients with CP have reduced bicarbonate secretion and decreased duodenal pH (normal pH 6.0-7.0, CP patients can lower to pH 4.0-5.0), further inhibiting pancreatic lipase activity (optimal pH 7.5-8.5);
Bile acid pancreatic enzyme synergy disorder: Pancreatic lipase needs to form mixed micelles with bile acids to function, and bile secretion may decrease in CP patients, exacerbating fat digestion disorders.
Digestive dynamics of fat diarrhea: from malabsorption to nutrient loss
Fat digestion requires the following steps:
Emulsification: Bile acids emulsify large particles of fat into small droplets, increasing surface area;
Hydrolysis: Pancreatic lipase hydrolyzes triglycerides into free fatty acids and monoglycerides;
Formation of mixed micelles: Free fatty acids, monoglycerides combine with bile acids and phospholipids to form mixed micelles;
Absorption: Mixed microglia enter the intestinal mucosal epithelial cells through the brush edges, re synthesize triglycerides, and package as chylomicrons into the lymphatic system.

Mechanism of Fat Diarrhea in CP Patients

CP patients may experience insufficient pancreatic enzyme secretion and changes in the duodenal environment, resulting in:
Incomplete fat hydrolysis: decreased pancreatic lipase activity, decreased triglyceride hydrolysis rate, and increased undigested fat in the intestine;
Formation barrier of mixed micelles: insufficient free fatty acids and monoglycerides, unable to effectively bind with bile acids;
Intestinal mucosal injury: Long term fatty diarrhea can lead to intestinal mucosal atrophy, further reducing the absorption area;
Bacterial overgrowth: Undigested fat provides nutrition for intestinal bacteria, and bacteria break down fat to produce metabolites such as hydroxy fatty acids, which inhibit intestinal mucosal absorption function.
In normal digestion, fat absorption mainly occurs in the upper segment of the jejunum (2-4 hours after eating). CP patients due to:
Delayed secretion of pancreatic enzymes: Fat hydrolysis is delayed to the middle and lower segments of the jejunum, where bile acid concentration is lower and the efficiency of mixed micelle formation decreases;
Accelerated intestinal peristalsis: CP patients often have diarrhea, shortened food passage time through the intestine, and insufficient contact time between fat and pancreatic enzymes;
Advance fat excretion: Undigested fat directly enters the colon, stimulating colonic peristalsis and increasing water secretion, leading to worsening diarrhea.

The mechanism of action of octreotide: a double-edged sword that inhibits pancreatic enzyme secretion
Octreotide Injection 100 mcg is an artificially synthesized octapeptide somatostatin analogue, whose functions include:
Inhibition of pancreatic enzyme secretion: By activating the somatostatin receptor (SSTR) on the surface of pancreatic acinar cells, inhibiting adenylate cyclase activity, reducing intracellular cAMP levels, and thus inhibiting pancreatic enzyme synthesis and secretion;
Inhibition of CCK release: Directly acting on SSTR in the duodenal and jejunal mucosa, reducing CCK secretion;
Regulating gastrointestinal motility: inhibiting gastric emptying and gallbladder contraction, delaying food entry into the duodenum;
Reduce portal pressure: Reduce blood flow by constricting visceral blood vessels, used to treat esophageal and gastric variceal bleeding.

Controversy over the role of octreotide in pancreatic enzyme silencing

Potential benefits of short-term inhibition of pancreatic enzyme secretion
Reduce pancreatic stimulation: CP patients may experience sustained high-level stimulation of the pancreas by CCK, and octreotide may alleviate pancreatic overstimulation and pain by inhibiting CCK release;
Reduce pancreatic juice secretion: Reduce the pressure of pancreatic juice on pancreatic ducts to prevent the formation of pancreatic pseudocysts or pancreatic fistulas.
The risk of long-term inhibition of pancreatic enzyme secretion
Aggravating pancreatic enzyme silencing: Octreotide may further inhibit the pancreatic enzyme secretion function of residual pancreatic acinar cells, exacerbating steatosis;
Interference negative feedback regulation: After octreotide inhibits CCK release, the concentration of trypsin in the duodenum decreases, which may promote CCK secretion through an unknown mechanism, forming a complex feedback loop of "octreotide CCK trypsin".

The indirect effect of octreotide on fat diarrhea

Delay gastric emptying and adjust the timeline of fat digestion
Octreotide inhibits gastric emptying and prolongs the residence time of food in the stomach, which may:
Delaying the entry of fat into the duodenum: providing more time for pancreatic enzyme secretion, but matching the pathological state of delayed pancreatic enzyme secretion;
Changing the location of fat digestion: If gastric emptying is delayed for too long, fat may directly enter the jejunum, missing the peak of pancreatic enzyme secretion.
Inhibit gallbladder contraction and bile acid secretion
Octreotide inhibits gallbladder contraction, reduces bile discharge, and may:
Exacerbating fat emulsification disorder: Insufficient bile acids directly affect fat emulsification;
Promoting the formation of gallstones: The incidence of gallstones in patients who use octreotide for a long time is as high as 15% -30%, which further interferes with bile secretion.
Regulating intestinal hormones and absorption function
Octreotide Injection 100 Mcg can inhibit the secretion of glucagon like peptide-2 (GLP-2), which promotes intestinal mucosal growth and repair. Inhibition of GLP-2 may exacerbate intestinal mucosal damage in CP patients, further worsening fat absorption.

Frequently Asked Questions
Can it be temporarily discontinued for 14 days? How long is the room temperature storage window?
+
-
Sure, it has a 14 day room temperature window. Unopened octreotide injection must be refrigerated (2-8 ° C) and stored away from light. But once taken out of the refrigerator, it can be stored stably at room temperature (<25 ° C) for up to 14 days and cannot be returned to the refrigerator. This provides convenience for patients who need short trips or temporary escape from the cold chain.
Why is the dosage required for treating "cancer like crisis" during surgery much lower than the instructions?
+
-
There is a possibility of individualized very low doses. In cancer like heart disease surgery, routine prophylactic infusion is 50-100 μ g/h. However, case reports have shown that when stubborn hypotension accompanied by facial flushing occurs during surgery, a shock dose of only 5-10 μ g (instead of the conventional 50-100 μ g) can quickly stabilize hemodynamics, and increasing the infusion rate to 200 μ g/h can control subsequent attacks. This indicates that with sufficient prevention, the dosage required to control acute attacks may be much lower than expected.
Can it make the gallbladder "lazy"? How long does it take to recover after stopping the medication?
+
-
Yes, it inhibits gallbladder contraction. Octreotide strongly inhibits the secretion of cholecystokinin, leading to weakened gallbladder contraction and bile stasis. A single injection can delay gallbladder emptying; After long-term low-dose treatment (about 500 μ g/day), stopping the medication can significantly restore gallbladder function within 2 weeks; However, for long-term treatment with high doses (about 1000 μ g/day), gallbladder emptying may still be delayed after 2 weeks of discontinuation.
Hot Tags: octreotide injection 100 mcg, suppliers, manufacturers, factory, wholesale, buy, price, bulk, for sale












