Pralidoxime Chloride Injection is an antidote used to treat organophosphate poisoning. It binds to the phosphoryl group in phosphorylated cholinesterase, freeing the cholinesterase and restoring it to its original state, thereby exerting its effect in rescuing organophosphate insecticide poisoning.
It has varying degrees of reactivation effect on the cholinesterase activity inhibited by acute organophosphate insecticides, but has poor toxic effects on malathion, dichlorvos, dichlorvos, dimethoate, mevalonate, propafenone, and octamethoxam. It has no reactivation effect on the cholinesterase activity inhibited by carbamate insecticides. Mainly used to rescue poisoning caused by various organophosphate insecticides. When used in combination with atropine, the dose of atropine should be reduced due to the enhanced biological effects of chlorpromazine. Atropinization should be maintained for 48 hours, gradually reducing the dose of atropine or extending the injection time thereafter.
At the same time, our company not only provides pure powders, but also tablets and injections. If needed, please feel free to contact us at any time.
 |
 |

Additional information of chemical compound:
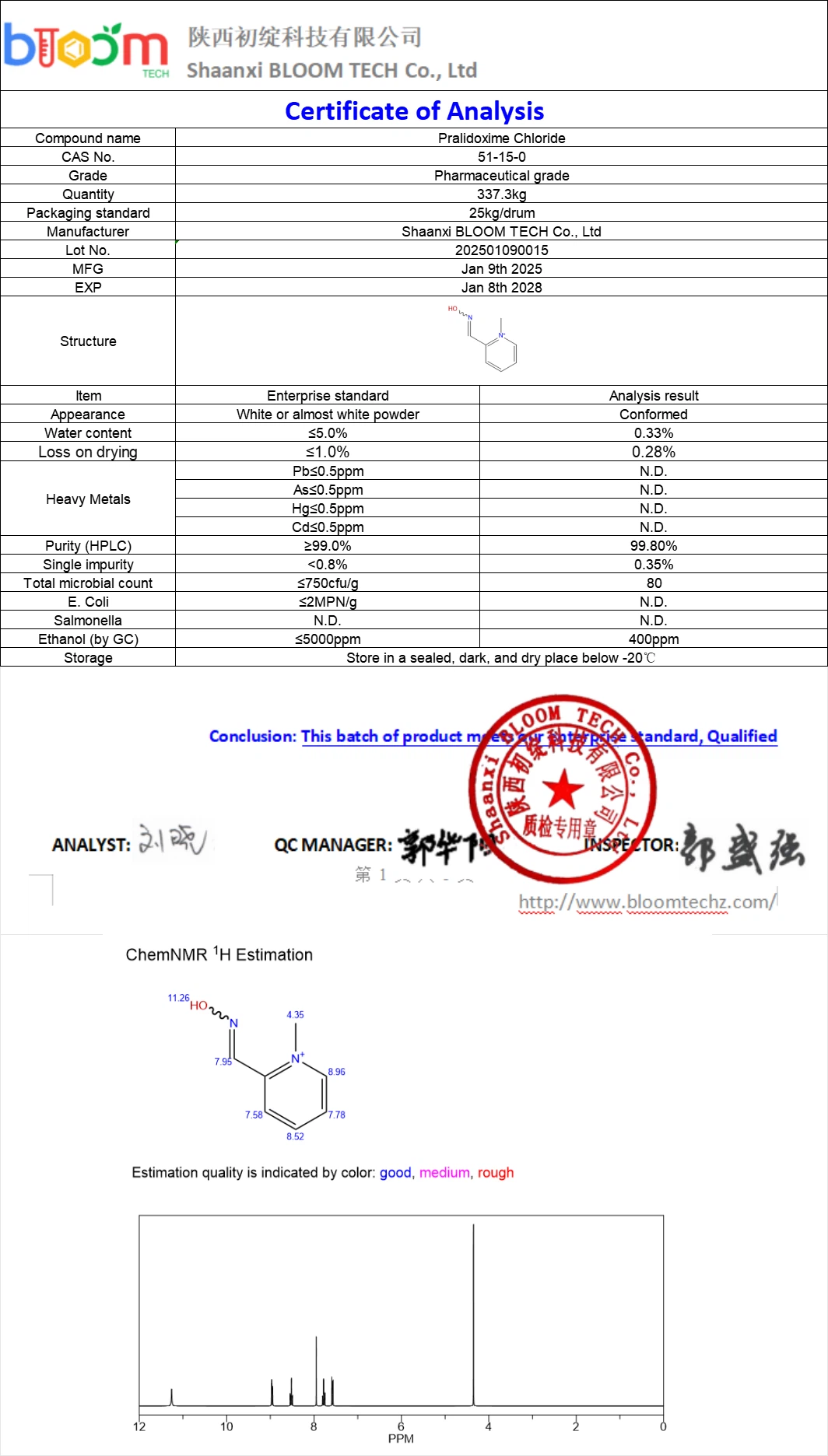
Pralidoxime Chloride COA


Pralidoxime Chloride Injection is an antidote used to treat organophosphate poisoning, and its dosage and administration need to be personalized according to factors such as the degree of poisoning, patient age, and weight. The following is a detailed introduction to the usage and dosage of Pralidoxime Chloride:
When adults suffer from mild organophosphate poisoning, the commonly used dosage of Chlorpromazine Injection is 0.4g/time to 0.5g/time. Usually diluted with glucose solution or physiological saline for intravenous infusion or slow infusion. If necessary, the medication can be repeated every 2 to 4 hours, and the specific frequency needs to be adjusted according to the patient's condition and blood cholinesterase level; When adults suffer from moderate organophosphate poisoning, the initial dose is usually 0.8g to 1.2g to quickly control the symptoms of poisoning. After the first administration, 0.4g to 0.8g can be given every 2 hours, for a total of 2 to 3 times; Alternatively, intravenous infusion can be used to maintain administration, with 0.4g administered per hour for a total of 4 to 6 times; When adults suffer from severe organophosphate poisoning, the first dose should be increased to 1g to 1.2g to quickly reverse the toxic state. If the symptoms do not improve after 30 minutes, an additional 0.8g to 1.2g can be given. Afterwards, 0.4g should be given every hour until the condition stabilizes.

Pediatric usage and dosage

The dosage of Chlorpromazine Injection for children is usually calculated based on body weight, usually 20mg/kg. When children suffer from mild organophosphate poisoning, chlorfenapyr injection can be administered at a dose of 15mg/kg, and repeated administration may be necessary. When suffering from moderate poisoning, the dosage can be increased to 20mg/kg to 30mg/kg, and the specific dosage needs to be adjusted according to the condition. When severely poisoned, the dose can reach 30mg/kg to quickly control the symptoms of poisoning. The administration method can be intravenous drip or slow intravenous injection.
Due to decreased function of organs such as the heart and kidneys, elderly individuals may have reduced tolerance to Pralidoxime Chloride Injection. Therefore, it is necessary to appropriately reduce the dosage and slow down the speed of intravenous injection during use. There is currently insufficient evidence to prove the safety of chlorfenapyr for injection in pregnant women and fetuses. Therefore, pregnant and lactating women should use it with caution and under the guidance of a doctor. For patients with liver and kidney dysfunction, the metabolism and excretion of chlorpromazine injection may be affected. Therefore, the dosage should be adjusted according to the condition during use, and the patient's liver and kidney function and blood drug concentration should be closely monitored.

Interaction with drugs
Pralidoxime Chloride Injection, as an antidote for organophosphate poisoning, mainly involves drug interactions with atropine and contraindications to compatibility with other drugs. The following is a detailed introduction:
Combination application and dose adjustment with atropine
Chlorfenapyr, as a acetylcholinesterase activator, can indirectly reduce the accumulation of acetylcholine and has a significant effect on the neuromuscular junction of skeletal muscles; Atropine directly antagonizes the accumulation of acetylcholine and has a strong effect on the autonomic nervous system. When the two are used in combination, they can jointly combat the pathological process of organophosphate poisoning through different mechanisms, significantly improving clinical efficacy. Due to the enhanced biological effects of atropine by chlorpromazine, the dosage of atropine should be reduced when used in combination to avoid adverse reactions caused by excessive inhibition of acetylcholine receptors.
Atropine dose adjustment plan:
|
|
|
|
Contraindications for compatibility with alkaline drugs: Chlorfenapyr is prone to hydrolysis reactions in alkaline solutions, producing inactive decomposition products that lead to reduced efficacy. Do not mix with alkaline drugs such as sodium bicarbonate to avoid drug degradation caused by pH changes. It needs to be separately configured with Chlorfenapyr Injection to avoid sharing the infusion channel with other drugs. Neutral solvents should be used during the preparation process to ensure that the pH value of the solution is maintained within the range of 5-7.
Differences in therapeutic efficacy compared to specific organophosphorus compounds: It has significant therapeutic effects on most organophosphate insecticides such as internally absorbed phosphorus and parathion poisoning. Restore nerve conduction function by reviving inhibited cholinesterase activity.
Cases with limited therapeutic efficacy. It has poor toxic effects on malathion, dichlorvos, dichlorvos, dimethoate, mevalonate, propafenone, and octamethoxam. There is no reactivation effect on acetylcholinesterase inhibited by carbamate insecticides.
Interaction with the aging state of cholinesterase: Inhibition of cholinesterase by organophosphate insecticides for 36 hours resulted in significant revival effect. The mechanism of efficacy attenuation is that after more than 36 hours, acetylcholinesterase undergoes an "aging" phenomenon, and the phosphorylated groups in its active center form stable covalent bonds with the enzyme protein, resulting in ineffective binding of chlorfenapyr. After being diagnosed with organophosphate poisoning, chlorfenapyr should be used immediately to avoid delaying treatment. Regular testing of blood cholinesterase activity is required. When the activity returns to 50% -60% of the normal value, adjustments to the medication regimen may be considered.
Interaction with symptoms of the central nervous system: It has a significant improvement effect on nicotine like symptoms (such as muscle tremors and muscle weakness), but has a weaker improvement effect on muscarinic symptoms (such as drooling and sweating) and central nervous system symptoms (such as coma and convulsions). According to the specific symptoms of the patient, atropine or other symptomatic supportive drugs should be used in combination. Establish comprehensive evaluation indicators including symptom scoring, cholinesterase activity, and vital signs.
Equivalent dose relationship with iodothyroxine: The content of oxime compounds in chlorfenapyr is 79.5%, significantly higher than the 51.9% in iodothyroxine. The efficacy of 1g Chlorfenapyr is equivalent to 1.5g Iodinapyr. Under the same therapeutic effect, the required dose of chlorfenapyr is smaller, which can reduce the injection volume and frequency. Lower doses can help reduce the incidence of drug-related adverse reactions.
Differences in response related to administration speed: The intravenous injection rate should be controlled at no more than 500mg per minute to avoid adverse reactions. Injecting too quickly can cause sympathetic nervous system excitement symptoms such as nausea, vomiting, and increased heart rate. In severe cases, central nervous system symptoms such as dizziness, headache, diplopia, blurred vision, and uncoordinated movements may occur. It is recommended to use intravenous injection for the first administration, and intravenous drip can be chosen for subsequent maintenance treatment. Use an infusion pump to precisely control the drug delivery rate and equip it with electrocardiogram monitoring equipment to monitor the patient's vital signs in real time.
General poisoning
The initial dose is 2-4mg, administered every 10 minutes via intramuscular or intravenous injection.
Severe poisoning
The initial dose is 4-6mg, administered every 5-10 minutes via intramuscular or intravenous injection.
Maintenance therapy
Atropinization needs to be maintained for 48 hours, after which the dose should be gradually reduced or the injection time extended.
Correlation with discontinuation indications
The main basis for discontinuing medication is the complete disappearance of nicotine like symptoms (muscle tremors, muscle weakness). The activity of blood cholinesterase should be maintained at 50% -60% or above of the normal value. Due to the slow absorption and long excretion cycle of organic phosphorus in the digestive tract, treatment needs to be maintained for 48-72 hours. Symptom assessment and cholinesterase activity testing should be conducted every 6 hours.
Synergistic effect with compound preparations
Compound Chlorfenapyr Injection (Chlorfenapyr Injection) is composed of Chlorfenapyr, Benazepine Hydrochloride, and Atropine Sulfate. Chlorfenapyr revives acetylcholinesterase activity, atropine antagonizes acetylcholine receptors, and benazepril enhances central anticholinergic effects. A single injection can achieve multiple treatment goals and reduce the frequency of nursing operations. By combining interventions with different targets, the success rate of treating organophosphate poisoning can be significantly improved.
Precautions for Elderly Individuals Using Pralidoxime Chloride
Special precautions for elderly patients using chlorpyrifos to ensure medication safety and efficacy:

Pre-administration Assessment
Allergy History Screening: Prior to administration, thoroughly inquire whether the elderly patient has a history of allergy to pralidoxime or organophosphate compounds. If severe allergic reactions (e.g., laryngeal edema, dyspnea) have occurred, contraindicate this medication to prevent anaphylactic shock.
Cardiovascular and Cerebrovascular Disease Assessment: Pralidoxime may induce cardiovascular reactions such as hypotension and tachycardia. Exercise caution when administering to elderly patients with hypertension, coronary heart disease, myocarditis, arrhythmias, or peripheral circulatory disorders. Strictly follow medical guidance to prevent exacerbation of underlying conditions.
Liver and Kidney Function Assessment: Chlorpyrifos is metabolized by the liver and excreted via the kidneys. Patients with impaired hepatic or renal function may experience drug accumulation. Evaluate liver and kidney function prior to administration. Adjust dosage or extend dosing intervals as necessary.
Monitoring During Administration
Vital Signs Monitoring: Closely observe heart rate, blood pressure, and respiratory rate to prevent respiratory depression or arrhythmias from overdose.
If respiratory depression occurs, immediately initiate artificial respiration and prepare emergency medications such as epinephrine.
Neurological Symptom Monitoring: Monitor for adverse reactions including dizziness, headache, blurred vision, double vision, or incoordination. Adjust dosage or discontinue promptly if observed.
High doses or prolonged use may cause severe central nervous system suppression, including epileptic seizures or coma. Immediately discontinue medication and seek medical attention.
Monitoring of Serum Cholinesterase Activity: Regularly test serum cholinesterase activity as a therapeutic monitoring indicator, maintaining levels above 50%-60%.
In acute poisoning cases, serum cholinesterase levels correlate closely with clinical symptoms. Close monitoring of clinical manifestations guides timely repeat dosing.

Frequently Asked Questions
What is the difference between atropine and pralidoxime?
+
-
Atropine will not act on the neuromuscular junction and has no effect on muscle paralysis or weakness, fasciculations or tremors; pralidoxime is intended to treat these symptoms. Systemic doses of atropine slightly raise systolic and lower diastolic pressures and can produce significant postural hypotension.
How quickly does pralidoxime injection work?
+
-
The onset time of Pralidoxime Chloride varies depending on the route of administration. When given intravenously, the effects can be observed within minutes. Intramuscular injection takes slightly longer to take effect, generally within 10 to 20 minutes.
Why is atropine not recommended?
+
-
Children or teenagers with congenital heart conditions may not be suitable for atropine treatment, owing to its potential influence on heart rate. Atropine eye drops could have increased side effects in children or teenagers taking medications which have a similar mode of action.
Who cannot take atropine?
+
-
Atropine generally is contraindicated in patients with glaucoma, pyloric stenosis, thyrotoxicosis, fever, urinary tract obstruction and ileus.
Hot Tags: pralidoxime chloride injection, suppliers, manufacturers, factory, wholesale, buy, price, bulk, for sale, CAS 1955546 93 6, 2 chloro 4 dibenzo b d furan 1 yl 6 phenyl 1 3 5 triazine, N1 1 1 biphenyl 4 yl N1 7 7 dimethyl 5 9 phenyl 9H carbazol 2 yl 7H benzo c fluoren 9 yl N3 N3 diphenylbenzene 1 3 diamine, 2 1 1 biphenyl 4 yl 4 spiro fluorene 9 9 xanthen 2 yl benzo h quinazoline, 4 bromo 9 9 dimethyl 9H fluorene, 7 4 4 5 5 tetramethyl 1 3 2 dioxaborolan 2 yl dibenzo b d furan 3 carbonitrile










